Marlus Stefanelli Heemann1; Francyne Veiga Reis Cyrino2
DOI: 10.17545/eoftalmo/2019.0006
ABSTRACT
Conjunctival myxoma is a rare neoplastic lesion, often confused with conjunctival cyst. This study reports a case of conjunctival myxoma initially diagnosed as conjunctival cyst, including the anatomopathological findings, and discusses the clinical importance of this diagnosis, due to its association with other diseases. In the two years of follow-up, the patient did not present recurrence after excision, even with conjunctival suture for scleral closure, and no comorbidities were observed.
Keywords: Conjunctiva; Diagnosis; Myxoma.
RESUMO
O mixoma conjuntival é uma lesão neoplásica rara, muitas vezes confundida com cisto conjuntival. Neste trabalho, é descrito um caso de mixoma conjuntival inicialmente diagnosticado como cisto de conjuntiva, seus achados anatomopatológicos e sua importância clínica devido à associação com outras patologias. Nos dois anos de seguimento, o paciente não apresentou recidiva após exérese mesmo com sutura de conjuntiva para o recobrimento escleral, assim como não apresentou associações com outras comorbidades.
Palavras-chave: Conjuntiva; Diagnóstico; Mixoma.
RESUMEN
El mixoma de conjuntiva es una lesión neoplásica rara, muchas veces confundida con quiste de inclusión conjuntival. En este trabajo, describimos un caso de mixoma de conjuntiva, inicialmente diagnosticado como quiste de inclusión conjuntival, sus hallazgos anatomopatológicos y su importancia clínica debido a la asociación con otras patologías. En los dos años de seguimiento, nuestro paciente no presentó reaparición después de la extirpación del mixoma con sutura de conjuntiva para el recubrimiento escleral, así como no presentó asociaciones con otras comorbilidades.
Palabras-clave: Conjuntiva; Diagnóstico; Mixoma.
INTRODUCTION
Myxomas are benign tumors derived from the primitive mesenchyme. They may present as isolated lesions or associated to syndromes such as McCune–Albright (intramuscular and cutaneous myxoma), Mazabraud (intramuscular myxoma), and Zollinger–Ellison (gastrointestinal schwannomas)1-3. These tumors are also observed in Carney complex, which includes cardiac and cutaneous myxoma, multiple pigmented lesions, and endocrine hyperfunction, with high morbidity and mortality. They can also be observed in skeletal muscles, bones, the gastrointestinal and genitourinary tract, and the nasal sinuses. Ocular involvement is quite infrequent, affecting the eyelids, conjunctiva, and orbit2.
Conjunctival myxoma is a rare ocular lesion, and approximately 40 cases are published in the literature. It predominantly affects adults, with no predilection for sex, and occurs more frequently in the left eye and temporal region. Among the conjunctival lesions, the incidence of this tumor was estimated to be 0.002% in a review of 2,455 patients1 and less than 0.001% in another study with 1,643 patients2. This condition is clinically and histopathologically distinct from extraocular myxomas; the differential diagnosis must include conjunctival cysts, amelanotic melanoma, amelanotic nevi, neurofibroma, lymphangioma, lipoma, and squamous-cell carcinoma, among others1-5.
Therefore, this study aimed to describe a lesion initially diagnosed as a conjunctival cyst, but proven to be conjunctival myxoma on histopathological analysis, as well as to discuss the disease evolution and the clinical relevance of the diagnosis.
CASE REPORT
A 41-year-old male, of black ethnicity, presented at our clinic complaining of a nodular lesion in the left eye, which had been increasing in size for approximately three years and caused pain on ocular movement. He had no history of ocular trauma and underwent a complete ophthalmologic examination. No alterations were observed apart from the findings in the left eye; the patient presented 20/20 vision in both eyes and the right eye presented no abnormalities.
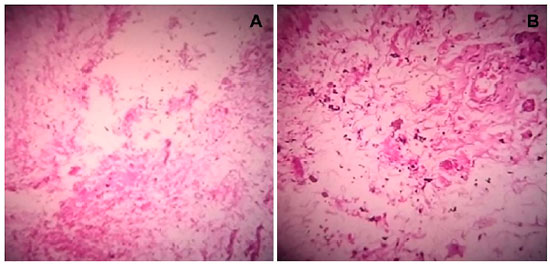
Biomicroscopy of the left eye indicated the presence of a raised, translucent, cystic, vascularized mass, measuring 8 mm × 7 mm (horizontal × vertical) in the temporal bulbar conjunctiva. Due to a clinical suspicion of conjunctival cyst, the lesion was removed under local anesthesia, the adjacent conjunctiva was dissected, and the temporal lesion was removed with safety margins. The conjunctiva was then sutured with mononylon 100. Histopathological examination described a macroscopic rounded mass of glossy, gelatinous grayish-brown tissue, measuring 0.8 × 0.6 × 0.3 cm; the microscopic analysis indicated a smooth myxoid stroma with cystic cavities and fusiform and star-shaped cells, compatible with a histopathological diagnosis of conjunctival myxoma (Fig. 1A and 1B). In light of this diagnosis, a systemic assessment was performed, ruling out cutaneous, cardiological, and endocrinological manifestations.
To date, at two years of follow-up, the patient did not present lesion recurrence or systemic manifestations (Fig. 2).
DISCUSSION
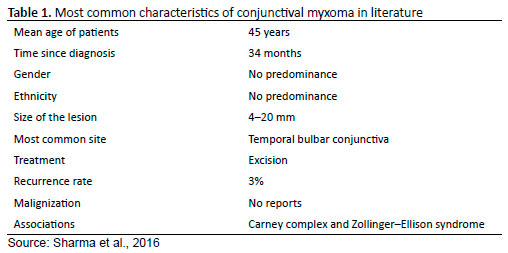
Conjunctival myxomas usually present as lesions of cystic appearance, with a fibrovascular component and soft tissue, of pinkish-yellow color, raised, and of slow growth until the diagnosis; in most cases, they are painless2,5. In a recent review of the literature, the mean age of the patients was 45 years and the mean time of lesion growth until diagnosis was 34 months; lesion size ranged between 4 and 20 mm in diameter, and most cases were observed in the temporal bulbar conjunctiva, similar to the present case3 (Table 1). Relapses are infrequent (3%), and there are no reports of malignancy in the literature3,5-7.
Conjunctival myxomas are not associated with other myxomas, such as those in McCune–Albright and Mazabraud syndromes; however, the literature describes a frequent association with Zollinger–Ellison syndrome (conjunctive myxomas + melanocytic schwannomas and pancreatic gastrinoma)8 and Carney complex. The latter is an autosomal dominant syndrome whose diagnosis requires at least two of the following criteria to be met: presence of myxomas, cutaneous punctiform nevi (conjunctiva, eyelids, lips, face, and trunk), and endocrine hyperactivity (Cushing syndrome, pituitary adenoma, and/ or sexual precocity). The ocular manifestations in Carney complex include lentigo of the eyelids, conjunctival or caruncle nevi, and conjunctival or palpebral myxomas. Thromboembolic events secondary to cardiac myxoma are observed in approximately 50% of patients with Carney complex. According to the literature, the onset of the ophthalmological manifestations associated with Carney complex may eventually precede these embolic events3,9.
In the present case, the conjunctival myxoma had a presentation similar to that described in the literature. The only unusual finding was pain on ocular movement, which is uncommon in these cases. Routine treatment is local surgical resection, usually without recurrence10. In the two years of follow-up after excision, the present patient did not present recurrence, even with conjunctival suture for scleral closure, and no comorbidities were observed.
CONCLUSION
Conjunctival myxoma is a benign lesion, but difficult to differentiate in clinical practice. Excision, followed by biopsy, is paramount and mandatory for the diagnosis of myxoma and other ocular conditions, allowing a correct diagnosis and appropriate treatment. The association with systemic syndromes indicates that patients with myxoma of the conjunctiva should undergo a clinical assessment.
REFERENCES
1. Grossniklaus HE, Green WR, Luckenbach M, Chan CC. Conjunctival lesions in adults. Cornea. 1987; 6(2):78-116.
2. Demirci H, Shields CL, Eagle RC, Jr, Shields JA. Report of a Conjunctival Myxoma Case and Review of the Literature. Arch Ophthalmol. 2006; 124(5):735-738.
3. Sharma, N, O’Hagan S, Phillips G. Conjunctival myxoma – atypical presentation of a rare tumour: case report and review of literature. BMC Ophthalmol. 2016; 16(1):54.
4. Pe’er J, Hidayat A. Myxomas of the conjunctiva. Am J Ophthalmol. 1986; 102(1):80-84.
5. Beggan C, Davies K, Leader M. Juxta-articular myxoma: an unusual benign mesenchymal lesion, readily mistaken for malignancy. Ir Med J. 2014; 107(7):212-213.
6. Patrinely JR, Green WR. Conjunctival myxoma: a clinicopathologic study of four cases and a review of the literature. Arch Ophthalmol. 1983; 101:1416- 1420.
7. Chen Y-P, Tsung SH, Lin TY-M. A rare presentation of conjunctival myxoma with pain and redness: case report and literature review. Case Rep Ophthalmol. 2012; 3:145-150.
8. Ramaesh K, Wharton SB, Dhillon B. Conjunctival myxoma, Zollinger-Ellison syndrome and abnormal thickening of the inter-atrial septum: a case report and review of the literature. Eye. 2001; 15(1):309-312.
9. Carney JA. The complex of myxomas, spotty pigmentation, endocrine overactivity and schwannomas. Semin Dermatol. 1995; 14(2):90-98.
10. Valles-Valles DR, Hernández‐Ayuso I, Rodríguez-Martínez HA, Medina-Cruz A, Salcedo‐Casillas G, Rodríguez‐Reyes AA. Primary conjunctival myxoma: case series and review of the literature. Histopatholog. 2017; 71(4):635-640.


Funding: No specific financial support was available for this study
Disclosure of potential conflicts of interest: The authors have no potential conflicts of interest to disclose
Received on:
October 23, 2018.
Accepted on:
February 18, 2019.